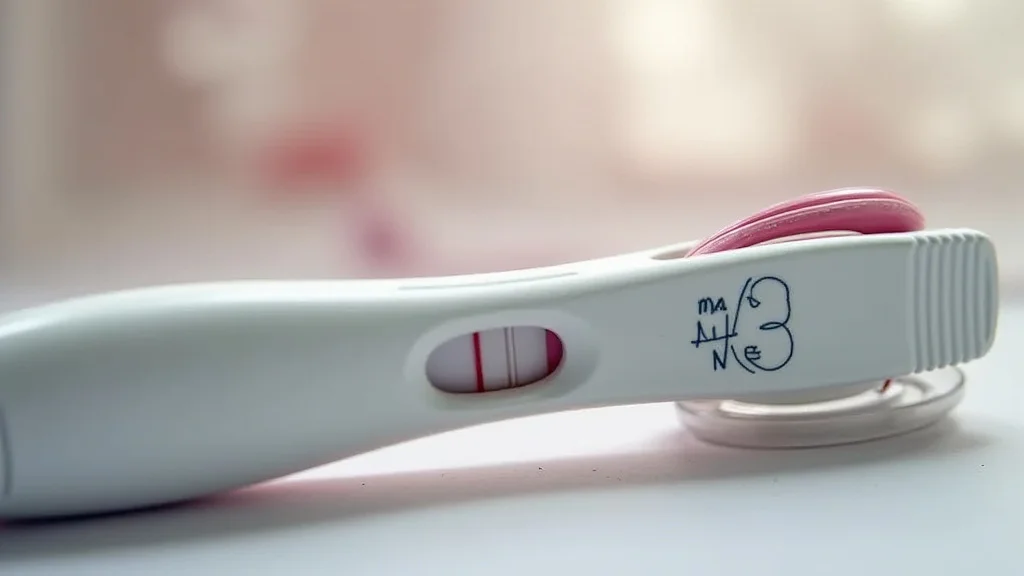
Figuring out which pregnancy test to buy can feel a little tricky at first. There are so many different ones, and it’s easy to get confused by all the names you see. But don’t worry!
This guide makes it super simple to learn about all the pregnancy tests names out there. We’ll go through it step by step so you know exactly what to look for. Get ready to feel confident about your choice!
Key Takeaways
- You will learn about the different types of pregnancy tests available.
- You will discover how pregnancy tests work to detect pregnancy.
- This post will clarify the meanings behind common terms used for pregnancy tests.
- You will understand how to choose the best pregnancy test for your needs.
- We will address common questions and myths about pregnancy tests.
How Pregnancy Tests Work
Pregnancy tests are designed to detect a specific hormone in your body. This hormone is called human chorionic gonadotropin, or hCG. Your body starts making hCG soon after a fertilized egg attaches to the uterine lining.
The amount of hCG grows very quickly in early pregnancy. Home pregnancy tests find this hormone in your pee or, less commonly, in your blood. When the test detects hCG, it shows a positive result, meaning you are likely pregnant.
The accuracy of the test depends on when you take it and how you follow the instructions.
The Role of hCG
Human chorionic gonadotropin (hCG) is a vital hormone produced by the placenta during pregnancy. It signals the body to maintain the uterine lining and support the developing embryo. hCG levels are very low before pregnancy.
They begin to rise rapidly after implantation, doubling approximately every 48 to 72 hours in the first trimester. Home pregnancy tests are specifically engineered to identify the presence of hCG in urine. The concentration of hCG in urine can vary depending on the brand of test and how many days it has been since your last period.
Some tests are more sensitive and can detect lower levels of hCG, allowing for earlier detection of pregnancy.
The scientific basis for detecting hCG involves antibodies that are sensitive to the hormone. When urine containing hCG is applied to the test strip, the hCG molecules bind to these antibodies. This binding triggers a chemical reaction that produces a visible line or symbol on the test.
This reaction is what gives you the positive result. The sensitivity of a test is often measured in milli-international units per milliliter (mIU/mL). A lower mIU/mL number means the test is more sensitive and can detect pregnancy earlier.
For example, a test with a sensitivity of 25 mIU/mL will need a higher concentration of hCG to show a positive result than a test with a sensitivity of 10 mIU/mL.
There are two main types of pregnancy tests: urine tests and blood tests. Urine tests are the ones you can buy at a drugstore and use at home. Blood tests are done by a healthcare provider in a lab.
Urine tests are convenient and provide quick results. Blood tests are more sensitive and can detect pregnancy earlier than urine tests. They can also measure the exact amount of hCG, which can be useful for monitoring a pregnancy.
Both types of tests rely on the detection of hCG to confirm pregnancy.
Detecting hCG in Urine
Urine pregnancy tests are the most common type used for home testing. These tests work by detecting the presence of hCG in your urine. When you take the test, you either dip the test stick into a cup of urine or hold the absorbent end in your urine stream for a specified amount of time.
The urine travels up the test strip via capillary action. If hCG is present in the urine above the test’s sensitivity level, it will bind to specific antibodies on the test strip. This binding causes a colored line or symbol to appear in a designated window on the test, indicating a positive result.
The control window shows a line that indicates the test is working correctly, regardless of the result.
The accuracy of a urine pregnancy test depends on several factors. The most important factor is the timing of the test. Testing too early, before your body has produced enough hCG, can lead to a false negative result.
It is generally recommended to wait until after you have missed your period for the most reliable results. Following the test instructions precisely is also crucial. For example, not allowing the test to sit for the recommended time or using urine that is too diluted can affect accuracy.
Many modern urine tests are over 99% accurate when used correctly and at the right time.
Some urine tests are designed to be digital, displaying the result as “Pregnant” or “Not Pregnant” words. Others show lines or symbols. The line tests might have two lines for pregnant and one line for not pregnant.
The interpretation of these lines can sometimes be confusing, especially if one line is fainter than the other. Digital tests are often preferred for their clear results, reducing any ambiguity. Regardless of the format, the underlying principle of detecting hCG remains the same.
Urine Test Accuracy Statistics
When used on the day of a missed period, home urine pregnancy tests are typically over 99% accurate. However, this high accuracy rate is based on using the test correctly and at the optimal time. If a test is taken too early, the accuracy can drop significantly.
For instance, if a test is taken four days before a missed period, the accuracy might be as low as 60-70%, depending on the test’s sensitivity. By the day of the missed period, this accuracy climbs to over 90%. A week after a missed period, the accuracy is generally considered to be virtually 100% for most standard tests.
Blood Tests for Pregnancy
Blood pregnancy tests are another way to detect pregnancy, but they are usually performed in a doctor’s office or a laboratory. There are two main types of blood tests: qualitative and quantitative. Qualitative tests simply detect whether hCG is present in the blood.
Quantitative tests, also known as beta hCG tests, measure the exact amount of hCG in the blood. This can be very useful for tracking the progression of a pregnancy or investigating certain pregnancy-related concerns.
Blood tests are generally more sensitive than urine tests. They can often detect pregnancy earlier, sometimes as soon as 6 to 8 days after ovulation. This is because hCG levels rise in the blood before they reach detectable levels in urine.
The quantitative blood test can also be used to estimate the gestational age of the pregnancy. As hCG levels rise rapidly in early pregnancy, the amount measured can give an indication of how far along the pregnancy is. Doctors may order serial quantitative hCG tests to monitor a pregnancy’s health, especially if there are concerns about miscarriage or ectopic pregnancy.
The convenience of home urine tests means most people use them first. However, for very early detection or when a more precise measurement is needed, a blood test is recommended. A positive blood test result is generally considered highly reliable.
A negative result may require retesting if pregnancy is still suspected, particularly if the test was done very early.
Common Pregnancy Tests Names Explained
When you go to the store or shop online, you’ll see many different brands and types of pregnancy tests. These often have distinct names, some of which hint at their features or how they work. Understanding these names can help you choose the right one for you.
Many are simply brand names, but others might refer to the test’s sensitivity or whether it’s digital. We’ll break down some common categories and names you might encounter, making the selection process much clearer.
Early Detection Tests
Many brands offer “early detection” pregnancy tests. These tests are designed to be more sensitive to hCG. This means they can detect pregnancy a few days before your expected period.
The names often include words like “Early,” “First Response,” or suggest a number of days, like “5 Days Sooner.” For example, “First Response Early Result” clearly states its purpose. These tests typically have a lower mIU/mL sensitivity, meaning they can pick up lower levels of hCG.
Using an early detection test can offer peace of mind sooner if you are trying to conceive or are concerned about a possible pregnancy. However, it’s important to remember that testing too early, even with an early detection test, can still result in a false negative. This happens if the hCG levels are not yet high enough for the test to detect.
If you get a negative result with an early detection test but still suspect you might be pregnant, it is wise to retest a few days later, closer to your missed period.
Statistics show that most women ovulate about 14 days before their period starts. Implantation typically happens about 6-12 days after ovulation. hCG production begins after implantation.
Therefore, an early detection test that claims to detect pregnancy 5 days before your period is likely detecting hCG around 9-10 days after ovulation. This requires a highly sensitive test strip. The earlier you test, the higher the chance of a false negative if implantation happened later than average or hCG levels are rising slower.
Examples of Early Detection Test Names
- First Response Early Result
- Clearblue Early Detection Pregnancy Test
- Pregmate Early Pregnancy Test Strips
- Accu-Clear Ovulation and Pregnancy Test
Digital Pregnancy Tests
Digital pregnancy tests are popular because they offer a very clear and easy-to-understand result. Instead of interpreting lines, these tests display words like “Pregnant” or “Not Pregnant” on a small screen. Names often include “Digital” or mention a clear display.
For instance, “Clearblue Digital Pregnancy Test” is a common example. These tests remove the guesswork often associated with interpreting faint lines on traditional tests.
The technology behind digital tests is similar to line tests; they detect hCG. However, the internal mechanism processes the signal from the hCG detection and translates it into a digital readout. This makes them a good choice for people who want a definitive answer without any confusion.
While often more expensive than standard line tests, the clarity of the results can be worth the extra cost for many individuals, especially during a time that can be emotionally charged.
It’s important to note that while the display is digital, the accuracy is still dependent on testing at the right time. Even digital tests should be used after a missed period for the most reliable results. Some digital tests also offer an option to estimate how many weeks pregnant you are, based on the detected hCG levels.
This feature can provide additional helpful information for those who receive a positive result.
Benefits of Digital Tests
- Clear, unmistakable results eliminate confusion.
- Reduces anxiety from trying to interpret faint lines.
- Some models offer pregnancy dating weeks since conception.
- Generally reliable when used at the appropriate time.
Pregnancy Test Strips
Pregnancy test strips are a very common and often the most affordable option. They are simple strips of paper that you dip into a collected urine sample. The names for these often include “Test Strips,” “Pregnancy Test Strips,” or might be part of a larger brand name like “Wondfo Pregnancy Test Strips.” They are known for their simplicity and cost-effectiveness, making them a popular choice for frequent testing or when multiple tests are needed.
To use test strips, you typically collect your first-morning urine in a clean cup. Then, you dip the absorbent end of the strip into the urine for a specific amount of time, usually a few seconds. After waiting for the recommended time, you place the strip on a flat surface and wait for the result, which usually appears as lines.
A control line indicates the test worked, and a second line indicates a positive result. The darkness of the second line can sometimes correlate with the level of hCG.
While economical, it’s crucial to follow the instructions carefully with test strips. Over-dipping or under-dipping can affect the accuracy. Also, using diluted urine can lead to a false negative.
Many people choose test strips because they can buy them in bulk at a lower cost per test. This is useful for people who want to test regularly, perhaps daily, as they wait for confirmation. The basic science is the same as other urine tests: detecting hCG.
Why Choose Test Strips
- Most affordable option available.
- Can be bought in larger quantities.
- Simple to use with a collected urine sample.
- Effective for early pregnancy detection when used correctly.
Pregnancy Test Kits
When people refer to “pregnancy test kits,” they are often talking about the complete packages you buy in a box at the store. These kits usually contain one or more test devices, along with detailed instructions. The name might be general, like “Home Pregnancy Test Kit,” or specify a brand and type, such as “e.p.t.
Pregnancy Test Kit.” These are complete, ready-to-use products designed for home use.
A typical pregnancy test kit will include the test device itself, which could be a stick with an absorbent tip or a midstream device that you hold under your urine stream. Crucially, it also contains a leaflet with instructions on how to use the test, how to read the results, and what the results mean. Some kits might include a urine collection cup, though many midstream tests do not require one.
The instructions are vital for ensuring accurate results. They detail how long to wait for the result and how to interpret the lines or symbols that appear.
The term “kit” simply implies that all necessary components for performing the test are included. It is a convenient way to purchase a pregnancy test as you don’t need to buy separate items like cups. Many kits are designed for single use, ensuring hygienic testing.
The reliability of the results from a kit depends heavily on following the included instructions precisely. Brands often invest in user-friendly designs for these kits to make the process as straightforward as possible for consumers.
What’s Typically in a Kit
- One or more test devices (sticks or strips).
- Detailed step-by-step instructions for use.
- Sometimes includes a urine collection cup.
- Information on interpreting results and next steps.
Choosing the Right Pregnancy Test
With so many pregnancy tests names and types available, selecting the right one can feel overwhelming. Consider what is most important to you. Are you looking for the earliest possible detection, the clearest results, or the most budget-friendly option?
Thinking about these factors will help you narrow down your choices. We will explore how to match your needs to the available test types.
Timing and Sensitivity
The most crucial factor in choosing a pregnancy test is often when you plan to take it. If you want to know as soon as possible, you need a highly sensitive test. These are often labeled as “early detection” tests.
They can detect lower levels of hCG, allowing you to test a few days before your missed period. A test sensitivity of 10 mIU/mL or 20 mIU/mL is considered high. A standard test might have a sensitivity of 25 mIU/mL or higher.
For example, if you are trying to conceive, you might want to use an early detection test around 10-12 days past ovulation. If you miss your period, using a standard test on the day your period is due is usually sufficient for an accurate result. Keep in mind that testing too early, even with a sensitive test, can still yield a false negative.
It is always best to follow the instructions on the packaging and retest if you get a negative result but still suspect pregnancy.
The chart below shows typical hCG levels and when tests can detect them. This helps illustrate why timing and sensitivity matter.
| Days Past Ovulation | Approximate hCG Level (mIU/mL) | Test Detectability |
|---|---|---|
| 8 | 0-10 | Not typically detectable by home tests |
| 10 | 5-50 | May be detectable by highly sensitive tests (e.g., 10 mIU/mL) |
| 12 | 20-100 | Most early detection tests can detect |
| 14 (Day of missed period) | 50-200 | Most standard tests (25 mIU/mL) can detect |
| 21 | 100-1000+ | Highly detectable by all tests |
Sensitivity Levels
- High Sensitivity (e.g., 10-20 mIU/mL): Best for early detection, a few days before a missed period.
- Standard Sensitivity (e.g., 25 mIU/mL): Accurate on or after the day of a missed period.
- Lower Sensitivity (e.g., 50+ mIU/mL): Less common for home use, may be used in specific medical contexts.
Readability and Ease of Use
The way a test displays its results and how simple it is to perform are also important considerations. If you prefer clear, unambiguous results, a digital pregnancy test might be the best choice. These tests eliminate any confusion about whether a line is faint or not.
The words “Pregnant” or “Not Pregnant” leave no room for interpretation.
On the other hand, traditional line tests are very common and often more affordable. If you are comfortable interpreting lines (a control line and a test line), these can be perfectly effective. Some people find the lines helpful because a fainter line might indicate lower hCG levels, suggesting very early pregnancy.
However, faint lines can also be confusing, leading to questions about accuracy. Test strips are generally very easy to use, requiring only dipping into a urine sample.
When choosing, think about your personal comfort level with interpreting results and the importance of immediate clarity. If you’re prone to anxiety, the straightforward nature of digital tests might offer more peace of mind. If budget is a primary concern and you don’t mind interpreting lines, standard tests or strips are excellent options.
Comparing Test Types for Ease of Use
- Digital Tests: Easiest to read results. Display clear words.
- Midstream Tests (Line): Easy to hold and use. Requires line interpretation.
- Test Strips: Simple dipping method. Requires urine collection and line interpretation.
Cost and Value
Pregnancy tests vary significantly in price. Test strips are typically the most inexpensive per test, often costing less than a dollar each when purchased in bulk. Standard midstream tests in a box usually cost a few dollars per test.
Digital pregnancy tests are generally the most expensive, sometimes costing $10-$20 or more for a single test. This higher cost often reflects the advanced display technology and the convenience it offers.
When considering cost and value, think about how many tests you anticipate needing. If you are testing frequently, especially in the early days of trying to conceive or before a missed period, test strips can be a very economical choice. You can buy large packs and test multiple times without spending a lot of money.
If you only need to test once or twice and want absolute clarity, a more expensive digital test might be worth the investment for the peace of mind it provides.
Always check the packaging to see how many tests are included in a kit. Sometimes a slightly more expensive box might actually contain two or three tests, making the per-test cost lower than a single, cheaper test. Reading reviews can also help you find tests that offer good accuracy for their price point.
Price Range Comparison
- Test Strips: Typically $0.50 – $2.00 per test.
- Standard Midstream Tests: Typically $3.00 – $10.00 per test.
- Digital Tests: Typically $10.00 – $25.00 per test.
Common Myths Debunked
There are many old wives’ tales and misconceptions about pregnancy tests. It’s important to rely on scientific evidence and manufacturer instructions for accurate results. Let’s clear up some common myths.
Myth 1: All pregnancy tests are the same.
This is not true. While most home pregnancy tests work by detecting hCG, they vary in sensitivity, format (lines vs. digital), brand, and price.
Some are designed for early detection, while others are standard. The quality and reliability can also differ between brands, so choosing a reputable one is important.
Myth 2: You can use any urine, anytime, for an accurate result.
For the most accurate results, it is generally recommended to use your first-morning urine. This is because hCG levels are usually most concentrated in the morning. Testing later in the day, especially after drinking a lot of fluids, can dilute your urine, potentially leading to a false negative result.
Always follow the specific instructions provided with your test.
Myth 3: A very faint line on a pregnancy test means it’s not accurate.
A faint line usually indicates that hCG is present in your urine, but at a lower concentration. This can happen when you are testing very early in pregnancy. As long as there is a visible line in the test window, it typically means the test is positive.
If you are unsure, retesting a few days later with a more sensitive test or your first-morning urine can help confirm the result.
Myth 4: You can test for pregnancy using household items like sugar or bleach.
These “DIY” or “at-home” remedies are not scientifically proven to detect pregnancy. They do not measure hCG levels. Relying on such methods can lead to inaccurate results and unnecessary stress or confusion.
It is always best to use commercially available pregnancy tests that are designed and tested to detect hCG accurately.
Frequently Asked Questions
Question: How soon can I take a pregnancy test?
Answer: Most home pregnancy tests can accurately detect pregnancy from the day of your missed period. Some highly sensitive “early detection” tests can detect pregnancy up to 5 days before your missed period, but accuracy is higher closer to your missed period.
Question: What is the difference between a qualitative and quantitative hCG blood test?
Answer: A qualitative hCG blood test simply tells you if hCG is present in your blood (yes/no). A quantitative hCG blood test measures the exact amount of hCG in your blood, which can be useful for monitoring pregnancy progress.
Question: Can taking certain medications affect a pregnancy test result?
Answer: Fertility drugs that contain hCG can cause a false positive result. Other medications usually do not affect the accuracy of most home pregnancy tests. Always check with your doctor if you are taking any medications and are concerned.
Question: What should I do if I get a positive pregnancy test result?
Answer: Congratulations! The next step is to schedule an appointment with your healthcare provider. They will confirm the pregnancy, usually with another test, and discuss your prenatal care options.
Question: Can a pregnancy test be wrong?
Answer: Yes, pregnancy tests can be wrong, leading to false positives or false negatives. False negatives are more common if you test too early. False positives are rare but can happen due to certain medications or medical conditions.
Summary
Understanding pregnancy tests names helps you pick the right test. Early detection tests find pregnancy sooner. Digital tests give clear word results.
Test strips are affordable and simple. Kits include everything you need. Choose based on when you want to test, how clear you need the result to be, and your budget.
Always follow the instructions for the most accurate results.